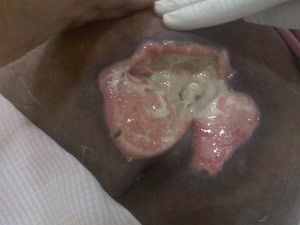
BEDSORES
History
They owe their origin to the observation that patients who were bedridden and not properly repositioned, would often develop ulcerations on their skin, usually over bony prominences. Such sores, which result from prolonged pressure, are also called
“decubitus ulcers” or “pressure ulcers/sores”.
Bedsores can develop within short periods – hours – and progress rapidly and are difficult to heal, till the inciting factor is removed.
So bedridden patients, paralyzed patients who cannot move by themselves or those who are unconscious and unable to feel the pain of sustained pressure are especially at risk.
Common Areas
Importantly bed sores do not always result from being in bed as the name implies. The location of the ‘bed sores’ usually depends upon the position of the patient.
For bed-bound patients, the sores are most likely to form on or around the lower back or tailbone – the commonest area in intensive care units -, the heels (especially in diabetics), & the hip-bone.
Pressure ulcers may also develop in a number of other areas, including the spine, ankles, knees, shoulders, and head, depending upon the position of the patient. Prolonged sitting may also contribute to formation of such ulcers especially in wheelchairs.